A new TV documentary reveals that superbugs are multiplying in the polluted wastewater flowing from pharmaceutical plants in India
Journalists from NDR and infectious disease researchers from the University of Leipzig travelled to India to investigate the runoff at pharmaceutical factories. In water samples collected in Hyderabad, a city known for its pharmaceutical industry, they found high concentrations of antibiotics as well as antibiotic-resistant bacteria. The results of this research were published last week in the scientific journal Infection.

To look for antibiotic-resistant bacteria the team of scientists and journalists took water samples from 28 different sites in Hyderabad, in November 2016. The samples were taken from tap and borehole water, and from environmental sites such as those near to pharmaceutical plants, as well as from a variety of rural and urban locations. The only sample which didn’t contain resistant bacteria came from a four star hotel.
After testing 16 samples for drug residues the team found that all of these environmental samples contained antibiotics or fungi. One sample stood out: a sample of water from a drainage channel contained an extremely high concentration of the fungicide fluconazole. The concentration of fluconazole in the sample was roughly a million times the recommended limit, and twenty times the concentration that is typically found in the blood of a patient being treated with the drug.
The scientists concluded that because the drug residue concentrations were so high, they most likely originated from pharmaceutical waste. Hyderabad is the central production site for antibiotics worldwide, and the team found that the city contained more than 40 pharmaceutical factories.

NDR Journalist Christian Baars
Tilo Gummel / NDR
The scientists can’t prove that the antibiotic residues in their water samples are what caused the bacteria in the samples to become resistant, because the resistant bacteria could also come from humans or animals who’ve been treated with antibiotics. However, it is obvious that the high concentrations of antibiotic residue in the environment „do not help“, said Christoph Lübbert, an infectious diseases expert at Leipzig University Hospital, who was one of the scientists on the team.
The new research also confirms the results of older studies, which have previously demonstrated both high concentrations of antibiotics and antibiotic-resistant bacteria in India (and reported on last October by Correctiv). NDR journalist Christian Baars, who worked on the new study, says that what is particularly novel about the new research are the findings relating to the fungicide fluconazole.
The research findings are very relevant to Europe, because antibiotic resistant bacteria in India are spreading globally and can be brought back tourists. Up to 90 per cent of people who travel to India return carrying resistant bacteria, scientists say, although in most cases the person will not become ill. Many of the drugs sold in Europe’s pharmacies are also made in either India or China, as a large proportion of antibiotics sold globally are produced in one of the two countries.
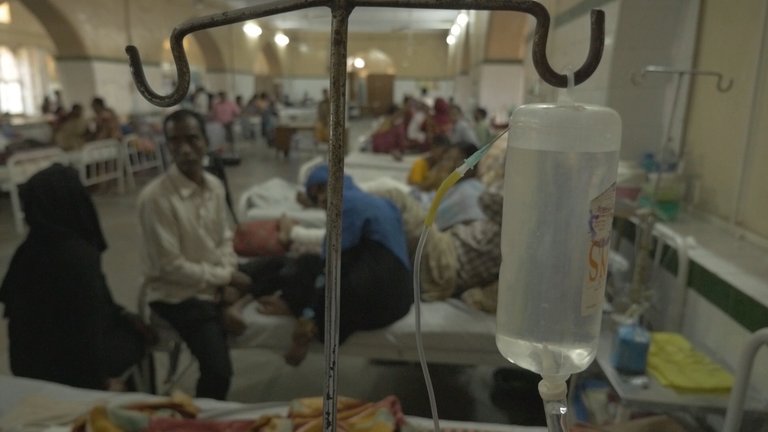
Osnmania Hospital in Hyderabad
Britta von der Heide / NDR
Critics are now demanding stricter environmental standards for imported medicines. This research provides enough reasons to demand better environmental standards, says Tim Eckmanns, head of the department of Nosocomial Infections at the Robert Koch Institute in Berlin. Although forcing pharmaceutical plants to produce less waste would not make the problem of antibiotic resistance disappear, he says, it would be a relatively easy way to reduce it.
The problem won’t disappear because there are other factors causing the number of resistant bacteria to rise, including over prescribing of antibiotics by doctors, and high consumption of antibiotics by livestock.
Reacting to the documentary, the German Federal Association of the Pharmaceutical Industry (BPI) said that the organization would take the report as an opportunity to „urge for a stricter compliance with agreed environmental directives“. But the industry „has no influence on the environmental standards set by the respective countries“, said Norbert Gerbsch, the CEO of BPI.
At EU level there are already regulations covering the „good manufacturing practice“ of imported drugs, but these only regulate the quality of the drugs and do not include environmental aspects.
Although one way of solving this could be to tighten controls and exclude manufacturers which do not limit their waste from the European market, this is not the way to solve the problem, Hermann Gröhe, Minister for Health (CDU), told the ARD. India and China must see that it’s in „their own interest not to endanger the effectiveness of the medical care of their large population,” he said.
Watch the documentary „The Invisible Enemy“ here, the work of a team from NDR, WDR and the Süddeutschen Zeitung.



